Journal Article:
Vasopressin V1a receptor is required for nucleocytoplasmic
transport of mineralocorticoid receptor
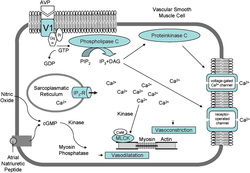
V1a receptor, used normally by vasopressin, or Antidiuretic Hormone, was tested to see if it had a direct correlation with aldosterone. Intercalated cells established from temperature sensitive, T antigen expressing rats were given either aldosterone or vasopressin, resulting in an increase in the nuclear to cytoplasmic ratio after 24 hours. These effects were accompanied by an increase in the expression of RCC-1 by aldosterone and a decrease in Ran Gap 1 (Ran GTPase activating protein) (Kahori Hori). Through a previous experiment, these researchers were able to deduce that the Vla receptor (V1aR) is essential for the acid-base regulation mediated by aldosterone, so there is a suggested cross communication between renin-angiotensin-aldosterone system (RAS) and the vasopressin system. In order to see if vasopressin would regulate aldosterone-induced transport of mineralocorticoid receptors, animal and cell cultures were used in order to investigate the hypothesis of vasopressin’s role in the regulation of the mineralocorticoid receptor (Kahori Hori).
VlaR knockout mice and intercalated cell line (IN-IC cells) were used. Fludrocortisone was injected into both wild and VlaR knockout mice for 3 days before the renal medulla was taken. The IN-IC cells were incubated at 33 degrees Celsius in a DMEM/F12 medium. In order to reduce other cell processes that are affected by vasopressin and aldosterone, antibodies against α tubulin, Brg-1, mineralocorticoid receptors, 11βHSD2, PKC, importin 7, Nup50, RCC-1 and Ran Gap were used (Kahori Hori). From this experiment, it was deduced that vasopressin V1aR is required for transport of mineralocorticoid receptor. Aldosterone stimulated the expression of the mineralocorticoid receptor and 11βHSD2 in the kidney (Kahori Hori). These effects were decreased in the V1aR deficient mice. Aldosterone dependently increased the expression of mineralocorticoid receptors over a 24-hour period. Vasopressin increased the protein and mRNA expression of MR over a 24-hour period (Kahori Hori). This shows that aldosterone and vasopressin work in conjunction in order to increase mRNA expression and that the VlaR receptor is needed by both aldosterone and vasopressin in order to stimulate the mineralocorticoid receptors
Another test was used to see if there was different stimulation of protein kinase c (PKC) pathways by vasopressin and aldosterone. This would show that V1aR would be a membrane-bound receptor of aldosterone. This hypothesis was rejected because vasopressin increased the expression of PKCα and –β1 in IN-IC cells, while aldosterone did not increase the expression of PKCα and –β1 (Kahori Hori). Also, vasopressin did not alter the expression of PKCδ or –ζ, but aldosterone did increase the expression of PKCδ and –ζ (Kahori Hori). This experiment inferred that vasopressin and aldosterone stimulate different PKC pathways, but the V1aR is essential for aldosterone’s action. An explanation for the dual use could be that luminal vasopressin may be required when aldosterone is released. The differences in the PKC pathways show that aldosterone and vasopressin independently regulate certain aspects of osmoregulation and volume regulation and that V1aR activates different PKC pathways when stimulated either by vasopressin or aldosterone.
The increase of production of RCC-1 and Ran Gap1 showed that vasopressin and aldosterone facilitate the transport of mineralocorticoid receptors in the nucleus (Kahori Hori). The lack of V1aR would cause a decrease in the decrease of RCC-1 and Ran Gap, but there would be further testing, according to the article. This research has shown that patients with chronic kidney disease, such as Addison’s disease, could have issues with mineralocorticoid receptors, and therefore the V1aR. There could be possible therapeutic usefulness of V1aR regulation. This article concluded that luminal vasopressin, which uses the V1aR regulates transports of mineralocorticoid receptors as well as some aldosterone receptors.
VlaR knockout mice and intercalated cell line (IN-IC cells) were used. Fludrocortisone was injected into both wild and VlaR knockout mice for 3 days before the renal medulla was taken. The IN-IC cells were incubated at 33 degrees Celsius in a DMEM/F12 medium. In order to reduce other cell processes that are affected by vasopressin and aldosterone, antibodies against α tubulin, Brg-1, mineralocorticoid receptors, 11βHSD2, PKC, importin 7, Nup50, RCC-1 and Ran Gap were used (Kahori Hori). From this experiment, it was deduced that vasopressin V1aR is required for transport of mineralocorticoid receptor. Aldosterone stimulated the expression of the mineralocorticoid receptor and 11βHSD2 in the kidney (Kahori Hori). These effects were decreased in the V1aR deficient mice. Aldosterone dependently increased the expression of mineralocorticoid receptors over a 24-hour period. Vasopressin increased the protein and mRNA expression of MR over a 24-hour period (Kahori Hori). This shows that aldosterone and vasopressin work in conjunction in order to increase mRNA expression and that the VlaR receptor is needed by both aldosterone and vasopressin in order to stimulate the mineralocorticoid receptors
Another test was used to see if there was different stimulation of protein kinase c (PKC) pathways by vasopressin and aldosterone. This would show that V1aR would be a membrane-bound receptor of aldosterone. This hypothesis was rejected because vasopressin increased the expression of PKCα and –β1 in IN-IC cells, while aldosterone did not increase the expression of PKCα and –β1 (Kahori Hori). Also, vasopressin did not alter the expression of PKCδ or –ζ, but aldosterone did increase the expression of PKCδ and –ζ (Kahori Hori). This experiment inferred that vasopressin and aldosterone stimulate different PKC pathways, but the V1aR is essential for aldosterone’s action. An explanation for the dual use could be that luminal vasopressin may be required when aldosterone is released. The differences in the PKC pathways show that aldosterone and vasopressin independently regulate certain aspects of osmoregulation and volume regulation and that V1aR activates different PKC pathways when stimulated either by vasopressin or aldosterone.
The increase of production of RCC-1 and Ran Gap1 showed that vasopressin and aldosterone facilitate the transport of mineralocorticoid receptors in the nucleus (Kahori Hori). The lack of V1aR would cause a decrease in the decrease of RCC-1 and Ran Gap, but there would be further testing, according to the article. This research has shown that patients with chronic kidney disease, such as Addison’s disease, could have issues with mineralocorticoid receptors, and therefore the V1aR. There could be possible therapeutic usefulness of V1aR regulation. This article concluded that luminal vasopressin, which uses the V1aR regulates transports of mineralocorticoid receptors as well as some aldosterone receptors.

This figure explains the effects of aldosterone and vasopressin on certain PKC subtypes. This figure contains eight graphs. Graph A shows the effects of vasopressin on PCKα for 15 minutes (Kahori Hori). The siRNA was at 1 while the control increased. In Graph B, aldosterone does not affect PCKα (Kahori Hori). The control and siRNA were at the same levels and the control decreased below the siRNA. In Graph C, vasopressin is used to increase PCKβ abundance (Kahori Hori). This was shown through the control being higher than siRNA. In Graph D, aldosterone is shown not having an effect on PCKβ abundance (Kahori Hori). Graph E shows that vasopressin does not effect the PCKδ (Kahori Hori). Graph F shows that aldosterone has an effect that increases PCKδ (Kahori Hori). Graph G shows that vasopressin does not have an effect on PCK –ζ (Kahori Hori). Graph H shows that aldosterone does have an effect on PCK –ζ abundance (Kahori Hori). This figure helps visualize PCK levels with the presence of either aldosterone or vasopressin. This also helps see the different roles of aldosterone and vasopressin.
Fig. 4
Fig. 4
